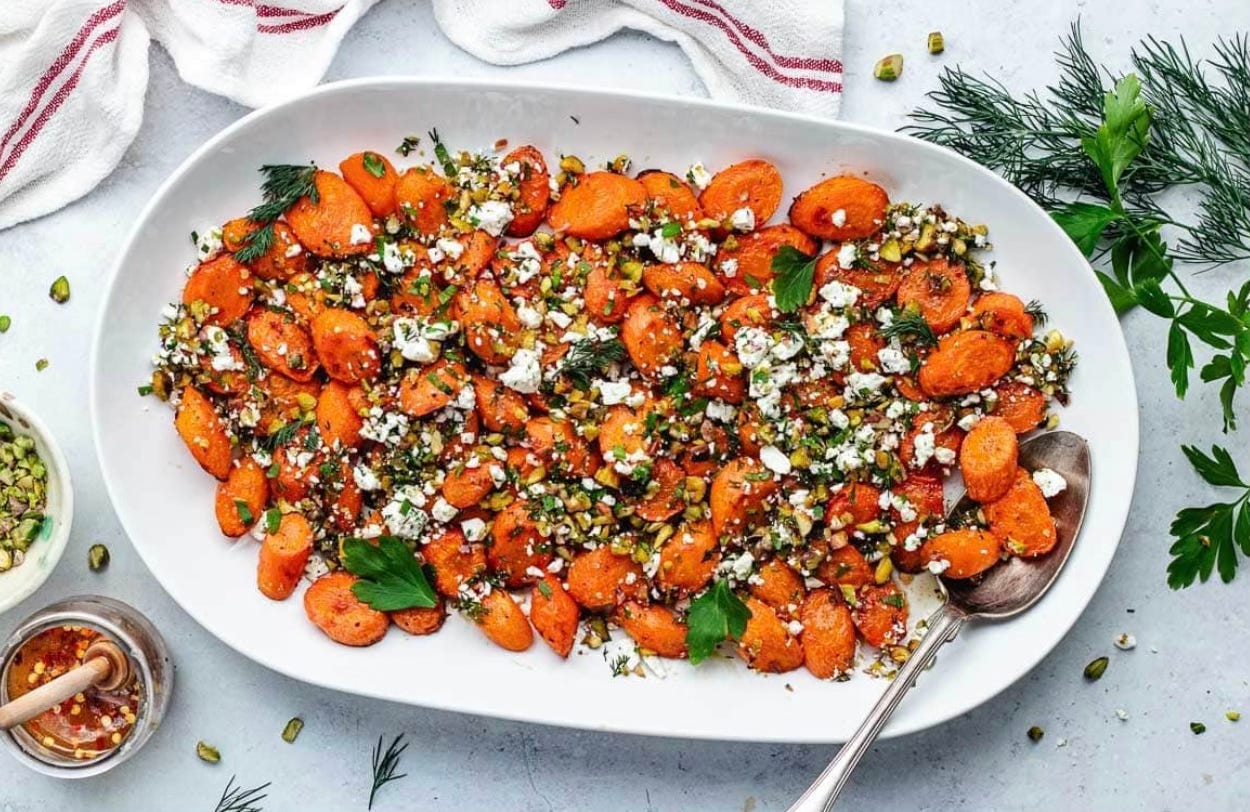Issue #98: head.ACHE.
hormonal headaches, hip pain in perimenopause, ginger, a spring herb garden, the other art fair, and new guidelines on endometriosis.
Did a friend send you this? Subscribe to receive our newsletter in your inbox weekly.
Headaches and migraines are a common—and often misunderstood—aspect of women’s health. While anyone can experience them, women are disproportionately affected, particularly during times of hormonal change. From the first menstrual cycle in puberty to the fluctuations of perimenopause, shifts in estrogen and progesterone can act as triggers, making headaches and migraines more frequent, severe, or cyclical. Recognizing this connection is key to identifying patterns and taking proactive steps to reduce both the intensity and frequency of episodes.
Cyclical migraines often align with the menstrual cycle, occurring just before or during menstruation when estrogen levels drop. Hormonal changes during puberty can spark the onset of migraines, and for many women, perimenopause can bring a resurgence or intensification as hormone levels fluctuate more dramatically. Beyond reproductive milestones, other triggers—stress, sleep disruption, diet, environmental factors, and even sensitivities to foods like gluten—interact with hormonal shifts, influencing headache frequency and severity.
By viewing headaches and migraines through the lens of women’s health, we can see them not as isolated events but as signals from the body. This perspective allows for more personalized strategies, combining lifestyle adjustments, dietary awareness, stress management, sleep support, and targeted natural interventions whether navigating puberty, perimenopause, or other hormonal transitions.
tips for reducing HEADACHES + MIGRAINES
Track Your Cycle & Headaches – Keeping a migraine/headache diary helps you identify patterns tied to hormonal shifts, food triggers, stress, and environmental exposures. Documenting when migraines occur can reveal if they’re linked to estrogen drops around your period or other triggers.
Elimination Diet to Find Food Triggers – Consider a 3–6‑week elimination diet where you remove common triggers (including caffeine, alcohol, aged cheeses, additives, and gluten) and then reintroduce one food at a time to see what provokes headaches. Gluten can be especially relevant for some—so testing for celiac or gluten sensitivity can be useful.
Eat Regular, Balanced Meals – Stabilizing blood sugar throughout the day reduces a common trigger for headaches and migraines, especially in people with insulin sensitivity or irregular eating patterns.
Hydration & Gut Health – Staying well‑hydrated is foundational, and supporting regular bowel movements with fiber (and possibly probiotics) can lower migraine frequency, as constipation has been linked with headaches in some cases.
Reduce Inflammation – A diet rich in antioxidants from fruits, vegetables, and anti‑inflammatory fats (like olive oil and omega‑3s) can help lower migraine triggers. Reducing sugar, processed foods, and inflammatory fats can also support long‑term prevention.
Supportive Supplements– Nutrients like riboflavin (vitamin B2), magnesium, fish oil (omega‑3s), and ginger (see below) have shown benefit in reducing migraine frequency and severity.
Acupuncture + Herbs– One of the most common things I see in the clinic are women experiencing headaches before/during their period. Acupuncture and herbs are great tools to reduce headache frequency and intensity and we can commonly address multiple symptoms of PMS at the same time.
Sleep + Stress Management – Regular sleep supports hormone balance and brain health, while stress reduction practices (meditation, yoga, breathwork) help lower overall migraine susceptibility.
Limit Environmental + Sensory Triggers – Bright or flickering lights, strong odors, loud noises, or changes in weather/pressure can set off migraines. Minimizing these exposures when possible is a key part of prevention.
Watch Medication Overuse – Frequent use of pain relievers can paradoxically cause medication overuse headaches. Reducing reliance on daily pain meds and working with a provider on safer prevention strategies can help break this cycle.
Hormonal Balance Strategies – Since shifts in estrogen (like during the menstrual cycle or perimenopause) can drop serotonin and lower pain thresholds—making migraines more likely—it may be helpful to discuss hormonal options with your provider. Need help finding one who is well-versed in hormonal therapy, send us a message!
save the DATE…we hope to see YOU!
click the images below for more details!
TASTE: Herbal Spotlight: Ginger. Warming, aromatic, and deeply rooted in traditional medicine, ginger (Zingiber officinale) offers more than digestive comfort—it’s increasingly supported by research for its role in pain, inflammation, and nausea. Studies suggest ginger may help reduce migraine severity and associated symptoms like nausea when taken at onset, while its anti-inflammatory compounds (gingerols) act on pathways similar to NSAIDs, offering a gentler option for some. It’s also well studied for dysmenorrhea, with evidence showing meaningful reductions in menstrual pain, and remains one of the most supported herbal remedies for nausea across contexts—from pregnancy to motion sickness. Ginger can be enjoyed fresh as tea or in food, or taken in capsule or tincture form for more consistent dosing; research-supported amounts typically range from 750–2,000 mg daily for menstrual pain and up to ~1–3 grams per day for broader therapeutic use, often divided throughout the day. While generally safe, higher doses may interact with medications like blood thinners, so individualized care matters.
BONUS TASTE: Roasted Carrots with Hot Honey, Pistachios, and Feta. I tried this recipe for Easter and everyone LOVED it! I used peanuts instead of pistachios (my dad is allergic to tree nuts)–the crumble and hot honey were so yummy! Next time you are looking for a side dish, give this one a try.
SEE: The Other ART Fair. Looking for something to do this weekend—and an excuse to head to Chicago? The Other Art Fair is back April 9–12 at Artifact Events, offering a refreshing, immersive take on the traditional art fair. With over 100 independent artists, the experience blends bold, accessible artwork with interactive installations, live music, and a social, come-as-you-are atmosphere—inviting you to connect directly with the artists and even start (or grow) your own collection. Part of a global series spanning cities like London, Los Angeles, Brooklyn, and Sydney, the fair is known for making contemporary art feel approachable and engaging. We’re especially excited to see our friend Cassandra Smith among the lineup, making it all the more worth the trip.
SMELL: The Ultimate Spring Project: An Easy Herb Garden. This guide makes a compelling case for starting a simple herb garden as the ultimate spring reset—less about perfection, more about reconnecting to scent, season, and daily ritual. Even a sunny windowsill can become a source of fresh aromatics like basil, sage, and lavender, bringing both flavor and fragrance into your space. The article emphasizes that success comes down to a few sensory basics: rich, well-draining soil, consistent (but not excessive) watering, and plenty of sunlight. There’s also something deeply satisfying about tending herbs from seed—watching them grow, pruning them to encourage more life, and using what you’ve nurtured in your kitchen or home. It’s a reminder that scent begins at the source, and that cultivating your own herbs is as much about slowing down and engaging your senses as it is about what ends up on your plate.
HEAR: ACOG Endometriosis Guideline Update. The recent update from the American College of Obstetricians and Gynecologists introduces new clinical guidance that supports earlier, symptom-based diagnosis of endometriosis using a combination of history, physical exam, and imaging—rather than requiring immediate surgical confirmation in all cases. This has sparked important—and at times heated—conversation within the endometriosis community. On one hand, the guidance aims to shorten the long delay to diagnosis by allowing clinicians to begin treatment based on symptoms and imaging, rather than requiring immediate surgical confirmation. For many, this represents progress: less invasive pathways, earlier validation, and faster access to care. On the other hand, advocates and specialists are pushing back on how the update is being interpreted and shared, emphasizing that laparoscopy with biopsy remains the gold standard for definitive diagnosis. They caution that imaging can miss disease, and that moving too far away from surgical confirmation risks underdiagnosis, delayed referrals, or over-reliance on symptom management without fully understanding disease severity. At the heart of the conversation is a shared goal—better, faster, more accurate care—but also a reminder that nuance matters, and how we communicate evolving guidelines can directly shape patient outcomes.
TOUCH: Years of Crossing my Legs + Perimenopause = Hip Pain. Speaking of aches, I’ve been having some hip pain this year, and guess what it is common! Turns out frozen shoulder isn’t the only joint-related issue that comes up in this phase of life. Gluteal tendinopathy is one of the most common causes of outer hip pain in women over 40 and often involves the gluteus medius (and sometimes minimus), showing up with things like side sleeping, walking, stairs, standing on one leg, or crossing your legs. I came across this post and am going to try and incorporate some of these exercises over the coming weeks. Research shows exercises like side planks, single-leg squats, RDLs, split squats, and single-leg bridges place high demand on the glutes and help rebuild strength over time. The goal is slow progression—finding movements that feel challenging and create fatigue without flaring pain.
What is appealing to your senses right now? What are you reading? watching? cooking? wearing? loving? obsessed with? We would love to share some of your picks in future newsletters!